

The study about the factors that affect the effect of nebulized inhalation by HFNC, among which VMN is more suitable for atomization inhalation therapy combined with HFNC.
When JN is used in combination with HFNC, the total gas flow in the HFNC system is greater than 6 L/min, which is also the minimum flow rate for running JN. This flow requirement limits the application of HFNC combined with JN nebulization inhalation in pediatric patients. Infants and young children often need HFNC gas flow less than 6 L/min. In addition, since the combination of HFNC and JN can cause changes in the oxygen concentration, total gas flow and pressure in the system, the integration of HFNC and JN is not necessarily appropriate.

In contrast, VMN is powered by electricity and does not require additional gas flow. In addition, the amount of drug residue in the JN nebulizer is higher than that in the VMN, with a JN residue of 45% and a VMN residue of only 3%. For children and adult patients, the inhaled drug dose produced by HFNC combined with VMN nebulization is generally 2 to 3 times higher than that of JN (Table 2). Therefore, compared with JN, VMN is more suitable for nebulized inhalation therapy in combination with HFNC.
HFNC gas is the "carrier" of aerosol. The gas flow, gas density and humidity of HFNC will affect the effect of nebulized inhalation.
For patients receiving HFNC, the total inhaled flow rate is a combination of the patient's inspiratory flow rate and the HFNC airflow rate. Any change in flow rate (flow rate) will affect the efficiency of nebulized inhalation. During quiet breathing, the amount of aerosol inhaled by HFNC combined with VMN is negatively correlated with the airflow of HFNC (Table 3). As the airflow rate increases, high-speed inhaled aerosol particles tend to form turbulence, and the aerosol will attenuate when passing through the trachea, bifurcation, and upper respiratory tract, and the amount of aerosol reaching the lower respiratory tract will continue to decrease. Therefore, there are guidelines that the flow rate should not be greater than 4 L/min when nebulizing children.
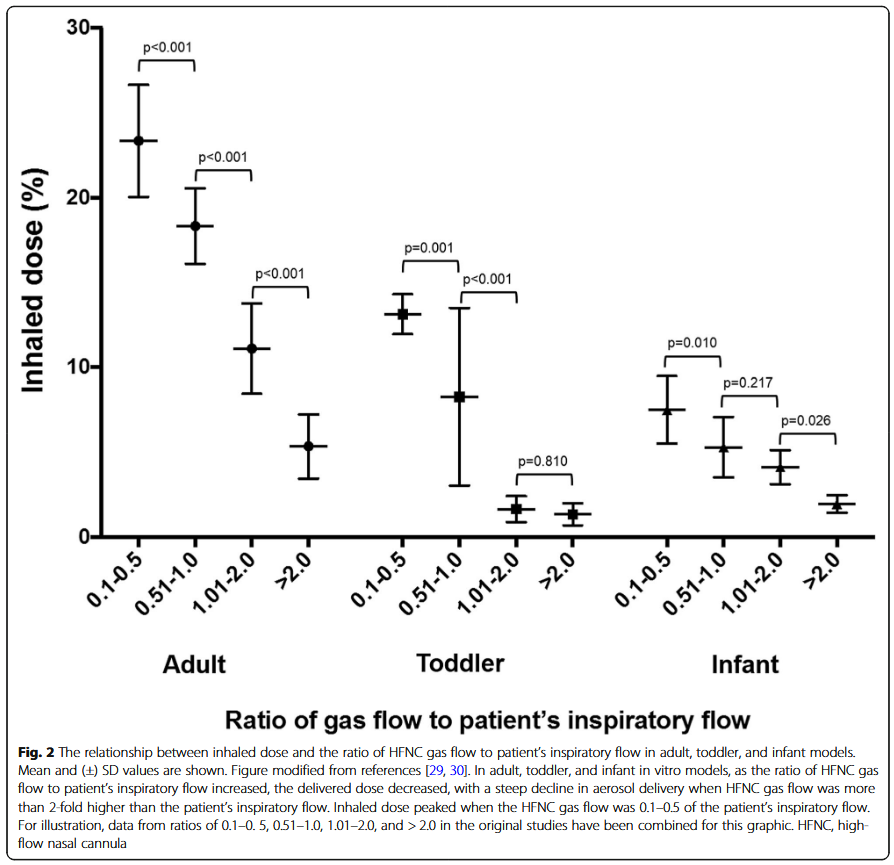
Two in vitro studies showed that in adults with dyspnea, the amount of aerosol inhaled increased when the HFNC airflow was reduced from 50 to 30 L/min, but decreased when the airflow was reduced to 10 L/min. When the HFNC airflow was 30 to 50 L/min, the amount of aerosol inhaled was greater than that of patients breathing quietly, but this was not the case when the airflow was 10 L/min. Subsequently, Li et al reported that the patient's inspiratory flow rate was more important than the set HFNC airflow rate. When the HFNC airflow was set to a lower than the patient's inspiratory flow rate, the amount of aerosol inhaled was greater than that set to a higher flow rate; when the HFNC airflow was set to 50% of the patient's inspiratory flow rate, the amount of aerosol inhaled was relatively constant. This result is consistent with the data for infants and children (Figure 2).
Currently, there is no commercially available device that can accurately measure a patient’s inspiratory flow rate during HFNC application. However, when clinicians administer nebulized therapy to a patient, monitoring the ratio of the patient’s inspiratory flow rate to the HFNC airflow can be used to titrate the HFNC airflow to produce the best clinical effect. A retrospective study of patients with pulmonary hypertension and hypoxemia found that bedside titration of airflow during nebulized prostacyclin via HFNC produced a better clinical effect than the use of a constant airflow.
Helium-oxygen (a mixture of helium and oxygen) has a lower density than oxygen or air and produces less turbulence when passing through narrow circuits/airways. For patients with severe airway obstruction, nebulized helium-oxygen can effectively reduce airway pressure and reduce gas trapping. A meta-analysis found that nebulized helium-oxygen can provide potential short-term benefits for children with moderate to severe pharyngitis. During HFNC, nebulized therapy with helium-oxygen as a carrier can reduce turbulence formation, thereby increasing aerosol dose.
For children and adults, nebulized helium-oxygen aerosol inhalation only shows a certain advantage when the airflow rate of HFNC exceeds the patient's inspiratory flow rate. Using helium-oxygen as an aerosol carrier just to improve the nebulization effect is not cost-effective, except for patients with severe airway obstruction, because helium-oxygen can effectively relieve dyspnea in such patients.
In vitro and in vivo studies in mechanically ventilated patients have shown that humidification reduces the amount of aerosol entering the lungs. Interestingly, during nasal nebulization at a flow rate of 30 L/min, Alcoforado et al. found that the inhaled dose of dry aerosol was 1-1.5 times that of humidified gas. Clinically, patient discomfort and potential adverse effects of dry aerosol inhalation at >6-10 L/min should be considered. In addition, during mechanical ventilation, turning off the humidifier 30 min before aerosol administration did not improve drug delivery efficiency. For these reasons, long-term delivery of aerosols using dry gases in non-humidified circuits is not recommended in clinical practice.
In vitro studies in pediatrics and adults have reported that aerosol deposition is greater when the VMN is placed at the humidifier inlet than when the nebulizer is placed close to the patient. Only in infants with very low airflow (0.25 L/kg/min) was the nebulizer more effective when placed closer to the patient. Because the VMN is placed farther from the patient, the carrier gas flow (including the delivery gas flow and the patient's inspiratory flow, plus a small tidal volume) may not be sufficient to deliver the aerosol to the patient before aerosol deposition occurs.
When the gas flow rate is higher than the inspiratory flow rate, adult studies have found that open mouth breathing reduces the inhaled dose compared with closed mouth breathing. This observation is consistent with a pediatric study report. Interestingly, when the gas flow rate is lower than the patient's inspiratory flow rate, open mouth breathing results in a higher inhaled dose than closed mouth breathing. Perhaps the aerosol collected in the nasal cavity at low gas flow during oral exhalation is inhaled during the next inhalation. Conversely, the higher gas flow flushes the aerosol out of the nasopharynx, reducing the amount of drug available for the next inhalation.